In 2014, the world’s largest-ever Ebola epidemic spread rapidly across West Africa, killing more than 11,000 people and infecting tens of thousands more.
Declared Ebola-free in June 2016, Guinea promptly set about strengthening its health system to prevent another outbreak, primarily by expanding the delivery of health services in rural communities. And the success of that strategy has been particularly apparent in the country’s progress against malaria, or, in French, paludisme.
Indeed, over the past five years, the government of Guinea has achieved impressive results in reducing the burden of malaria, including a sharp decline in malaria prevalence among children under five, substantially reduced annual incidence, and fewer inpatient deaths. And it’s done so in large part through StopPalu, a project launched in 2013 with funding from USAID under the U.S. President’s Malaria Initiative (PMI).
Implemented by RTI International in 14 of the country’s districts (préfectures) and the five communes of the capital, Conakry, StopPalu employed a community-driven approach to promote the prevention, diagnosis, and treatment of malaria, one of the leading causes of illness and death in Guinea.
Under StopPalu, RTI helped train more than 1,400 volunteer community health workers (CHWs) on a set of skills collectively known as “malaria community case management.” Trained on the use of rapid diagnostic tests, CHWs first confirm whether a patient with a fever has malaria. And for those who test positive, CHWs are trained to administer artemisinin-based combination therapy, or ACT, and to refer severe malaria cases to health facilities.
Now, under StopPalu+, a follow-on of StopPalu launched in December 2017 that targets the same geographic areas, RTI continues to support Guinea’s National Malaria Control Program as it builds on that success, notably with the rollout of an ambitious campaign to distribute long-lasting insecticidal nets, or LLINs. The third such campaign since 2013, and Guinea’s largest ever, it’s a testament to forward-looking leadership and cooperation among a diverse group of stakeholders, who worked together to achieve a common goal.
Insecticide-treated Bednets: The First Line of Defense
On April 25, World Malaria Day, throngs of revelers in the city of Fria gathered to celebrate the launch of the campaign at a joyous ceremony in the central stadium. Chaired by Guinea’s Minister of Health, Dr. Edouard Nyankoye Lamah, the event resembled something between a pep rally and a military parade, with boisterous singing, trumpets and snare drums, ensembles of dancers twirling in bright red skirts and rows of soldiers standing at attention in crisp green uniforms.
In a speech from the grandstand, U.S. Ambassador to Guinea Simon Henshaw praised the country’s “extraordinary progress” against malaria while also cautioning against complacency.
“On the occasion of World Malaria Day and the launch of the LLIN distribution campaign, the U.S. is proud to partner with Guinea in its efforts to defeat this disease,” he said in French. “And we salute the heroes of Guinea’s health sector: the doctors, nurses, community health workers, laboratory technicians, pharmacists, researchers, mobilizers, drivers, storekeepers, data entry specialists and many others who work to protect health and prevent illness.”
Still, Henshaw said, much remains to be done: “Diverting our attention will result in a resurgence of malaria-related morbidity and mortality, jeopardizing the substantial investments made to date.” As the world’s largest global health donor, he added, the U.S. remains strongly committed to the fight—in Guinea and around the world. “We are ready to defeat malaria. Are you?”
Together, Henshaw and Lamah formally kicked off the bednet distribution campaign with the ceremonious presentation of Fria’s first net, handing it over amid the clicking of cameras to a mother of three. By July 2019, the campaign distributed some 3.45 million nets to more than one million households in the area covered by the project, putting in people’s hands a cornerstone of malaria control.
Widely considered one of the most effective tools for reducing malaria transmission, bednets serve as an essential first line of defense. It’s estimated that—due to its property as a physical barrier between mosquitoes and users as well as the insecticide on it that kills mosquitoes—the use of bednets accounts for nearly 70 percent of malaria cases averted in Africa since 2001. The World Health Organization has issued new guidance calling for “universal coverage.” The agency now recommends that bednets be distributed for free to all people in malaria-affected areas, not just the most vulnerable groups (pregnant women and children under five), and that campaigns should utilize multiple channels, including antenatal clinics, schools, and faith-based networks.
Mass distribution may sound simple in principle: procure bednets and pass them out to everyone. But the devil is in the details—the transport and the storage, the enumeration of households, training on distribution activities and social mobilization, the monitoring and multi-level supervision, the media coverage, the budget development, and the critically important dissemination of key messages.
There is so much that goes into it before even a single net is distributed,” says Dr. Aissata Fofana, chief of party for StopPalu+, who for years has criss-crossed the country, forging relationships with the many community leaders vital to any campaign’s success. “You have to prepare and prepare, because it isn’t just making the nets available—it’s ensuring that everyone uses them correctly and regularly.
The morning after the ceremony in Fria’s central stadium, Fofana visited one of the city’s main distribution sites. By the time she arrived, the team of StopPalu+ volunteers was in place, and a line of people stretched around the block—dozens of men and women waiting in the sun, many with young children in tow.
All were holding the paper vouchers they’d received weeks earlier when StopPalu+ enumerators came to count the members of each household. The enumerators had recorded each member’s name and age, and they’d written on the back of the voucher the date and location of the distribution. “No voucher, no net,” they’d warned, urging people to store it in a safe place.
“I demonstrate how to hang the nets, how to wash and repair them, and how to reduce the potential side-effects of the insecticide,” said Mariama Bah, one of five StopPalu+ volunteers assigned to the distribution site. “People don’t always know that the bednet can be used on all types of sleeping spaces, and that they should be used throughout the year by everyone in the household, even when they’re sleeping outside.”
Linking Malaria Control with Maternal Health
One devastating effect of the Ebola epidemic was the erosion of confidence in Guinea’s health system. Fearing infection, many in Guinea stayed away from health facilities, and long after the epidemic had been brought to an end, that fear lingered, leaving many at heightened risk of illness and death.
Particularly vulnerable were pregnant women. Because pregnancy reduces a woman’s immunity to malaria, pregnant women are more susceptible to infection and more likely to suffer from severe anemia than their nonpregnant counterparts.
Guinea’s Ministry of Health believes that by creating strong linkages with maternal and child health services, it can multiply malaria prevention and treatment results, providing greater protection for those least able to protect themselves. And with PMI support, the government is doing just that, delivering key malaria interventions through routine antenatal visits, including the continuous distribution of bednets.
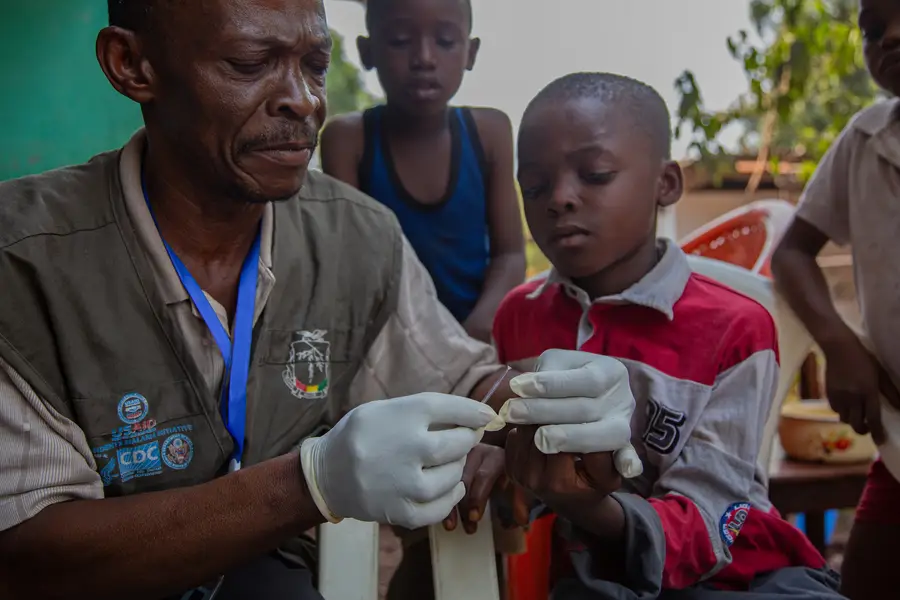
During a home visit in Sabendé, a village on the outskirts of Fria, Lamine, one of 2,000 StopPalu+-trained community health workers, took a finger-prick blood sample from a boy with a fever and ran a rapid test for malaria. As they waited for the results—the test takes about 15 minutes—Lamine encouraged the boy’s pregnant mother to attend her antenatal care visits at the clinic in town and to continue sleeping under a bednet even after she delivers. “Malaria is even more dangerous for you,” he told her. “Pregnant women have to be especially careful.”
Lamine first started working with StopPalu when, he says, “there was so much malaria.” But in the time since, he says, things have gotten better. He now finds fewer cases in his community and more people using bednets. And seemingly everywhere, he says, even in the villages farthest from Fria, people know StopPalu+. “When they see me coming, they give me a warm welcome,” he says, smiling. “They know I’m there to help, and that’s what I do.”