Evaluating the Accountable Health Communities (AHC) Model to test whether connecting people to community resources to address nonmedical needs such as food insecurity and housing instability can improve health outcomes and reduce costs
The final evaluation report showed that the AHC Model generated over $200 million in savings.
The conditions in which people are born, grow, work, live, and age are increasingly recognized as important drivers of their health and well-being. These conditions are just as important—if not more so—as clinical care for determining health outcomes.
Addressing Factors That Impact Health Outcomes
Targeting underlying community-level economic conditions or individual-level needs, such as food insecurity and housing instability, can improve overall health outcomes. For both community-level and individual-level strategies, data are critical to
- Documenting factors that make it difficult to access care
- Identifying individuals and communities who are at a higher risk
- Designing effective policies and interventions
- Measuring whether the policies and interventions improve health outcomes.
However, the data needed for those strategies are often lacking. The Accountable Health Communities (AHC) Model was a major Centers for Medicare & Medicaid Services (CMS) initiative that aimed to fill this gap. The AHC Model tested whether screening Medicare and Medicaid beneficiaries for core needs (food, housing, transportation, utilities, and safety) and using navigators to connect qualified beneficiaries to community resources to address these core needs can improve health outcomes and reduce costs. (Qualified beneficiaries had at least one core need and at least two emergency department visits in the year before screening.)
Evaluating the Accountable Health Communities Model
As the evaluator of the AHC Model, RTI International analyzed rich data from model participants. These data provide information about (1) whether any of the five core needs are prevalent among screened Medicare and Medicaid beneficiaries; (2) whether beneficiaries were successfully connected to community resources; and (3) whether their needs were resolved.
We utilized a mixed methods evaluation design to
- Understand how the AHC Model was implemented
- Assess success in connecting beneficiaries to community resources and resolving their needs
- Measure impacts on health care utilization and expenditures
- Understand how implementation and contextual factors are associated with model impacts.
The evaluation drew on various data types and sources—including model participant data, publicly available data to describe community context, fee-for-service claims and Medicare Advantage encounters for Medicare beneficiaries, Transformed Medicaid Statistical Information System (T-MSIS) data for Medicaid beneficiaries, key informant interviews, and beneficiary and organizational surveys. To evaluate health care utilization and expenditure impacts, we took advantage of random assignment of beneficiaries to the model intervention in some areas; in other areas, we utilized quasi-experimental difference-in-differences analysis.
Understanding the Findings
The final evaluation report showed that the AHC Model generated over $200 million in savings after accounting for CMS investments. These savings were generated by significant reductions in inpatient stays and emergency department visits, which drove reductions in total Medicaid and Medicare expenditures. Interviews with AHC Model stakeholders revealed a positive impact on their engagement with the health care system. By fostering trust, navigators were able to effectively empower beneficiaries to be more proactive in seeking suitable care, which potentially decreased the need for acute care services. This finding underscores the importance of personalized assistance and highlights the potential of navigation services in bridging the gap between health care services and individuals who have difficulty accessing care.
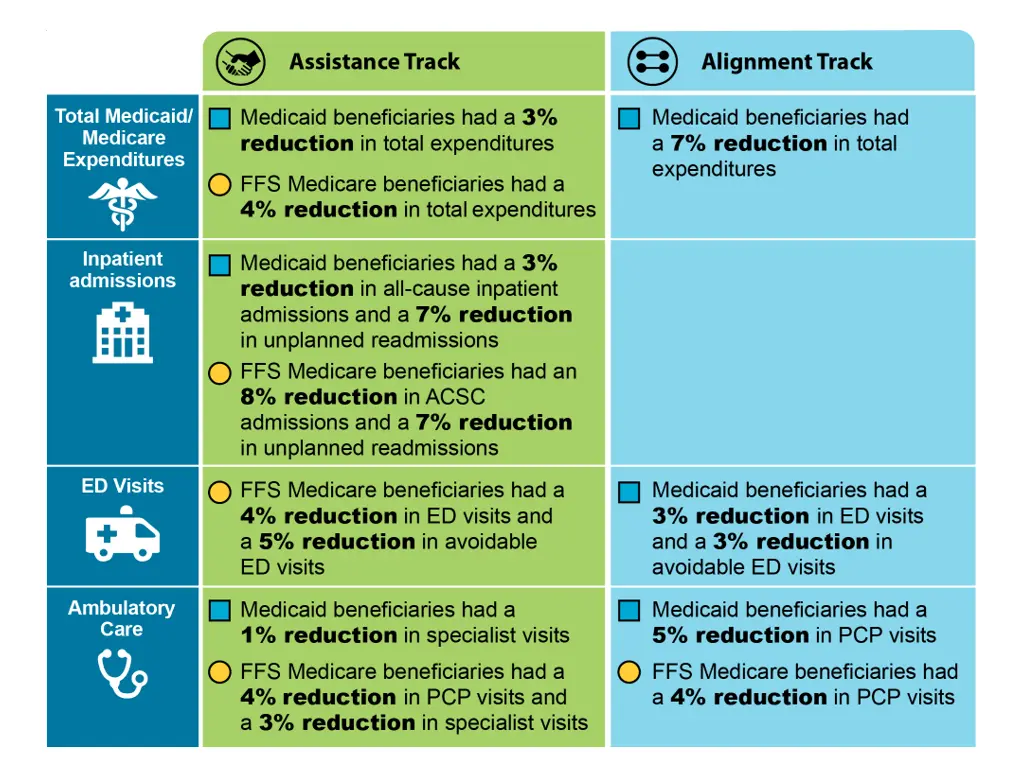
Definitions: ACSC = ambulatory care sensitive condition; ED = emergency department; FFS = fee-for-service; PCP = primary care provider.
Note: The infographic only highlights impacts that were statistically significant.
Moving Forward: Using Data to Improve Health Outcomes
The Accountable Health Communities Model has shown promise in enhancing health care outcomes. The reductions in acute care services and expenditures signifies its positive impact on patient outcomes and resource allocation. As the health care landscape evolves, the AHC Model serves as a prototype for change, inspiring a patient-centered and holistic approach that addresses the underlying drivers of health.
Learn More
For more about this project, visit the CMS Accountable Health Communities (AHC) Model Evaluation page.
- Center for Medicare and Medicaid Innovation (CMMI)
- Abt Associates
- Social Interventions Research & Evaluation Network (SIREN) at the University of California San Francisco
- Inciter





