As outlined in the last blog in our series “The Time is Now: Investing in Adolescent Health", there is a huge need to address poor mental health among adolescents. An estimated 80% of adolescents in need of mental health services do not receive care, although the true number is likely higher in low- and middle-income countries (LMICs).
The urgency of addressing this burden has been heightened by recent experiences with COVID-19, growing alarm about environmental issues, and new learnings about the impact of social media and technology use. As school-closures and lockdowns, due to COVID-19, have disrupted the lives of adolescents around the world, routines and relationships have been under strain. Some young people have also experienced hardship resulting from the economic impacts of COVID upon their families.
A survey conducted by UNICEF in Latin America and the Caribbean found 27% of young people reported anxiety and 15% reported depression. In the survey, 30% of young people reported that the biggest reason for their current emotions was their economic situation. More evidence is needed, particularly from LMICs, but there are strong indications that a higher than usual number of young people may be experiencing poor mental health as a result of the pandemic.
Additionally, concerns about environmental issues, particularly climate change, environmental degradation, and biodiversity loss, are increasingly at the forefront of the minds of young people, and have been indicated to contribute to stress, anxiety, and contributing to poor mental wellbeing.
Finally, emerging evidence has highlighted the negative impacts of social media on the mental health of young people, with more frequent social media use and high screen time linked to increased risk of anxiety and depression.
The Economic Case for School-based Mental Health Interventions
School-based health programs and services are an important approach that harness existing systems to reach a large population of young people. These inter-sectoral partnerships are particularly promising for programs targeting prevention and can be an effective way to reach adolescents who may not otherwise access health services due to stigma or other barriers such as cost, location, or age restrictions.
Sexual and reproductive health, nutrition, and de-worming programs have successfully been implemented through schools in many countries. Evidence from high-income countries suggests schools are also a promising setting for mental health promotion. While these programs exclude adolescents who do not attend school, they are a valuable platform for addressing mental disorders and scaling up access to services that are currently inaccessible for many adolescents in LMICs.
RTI has been working on adolescent mental health in partnership with the AstraZeneca Young Health Programme (YHP) since 2017. As part of this effort, we analyzed the return on investment (ROI) of a package of school-based mental disorder prevention interventions for the newly released UNICEF 2021 State of the World’s Children report.
The package of interventions we analyzed includes programs to prevent anxiety, depression, and suicide among adolescents, which were chosen because they have been demonstrated to be both effective in improving health outcomes and cost-effective to deliver. Participation in these programs is associated with decreased risk of developing anxiety and depression and of dying by suicide.
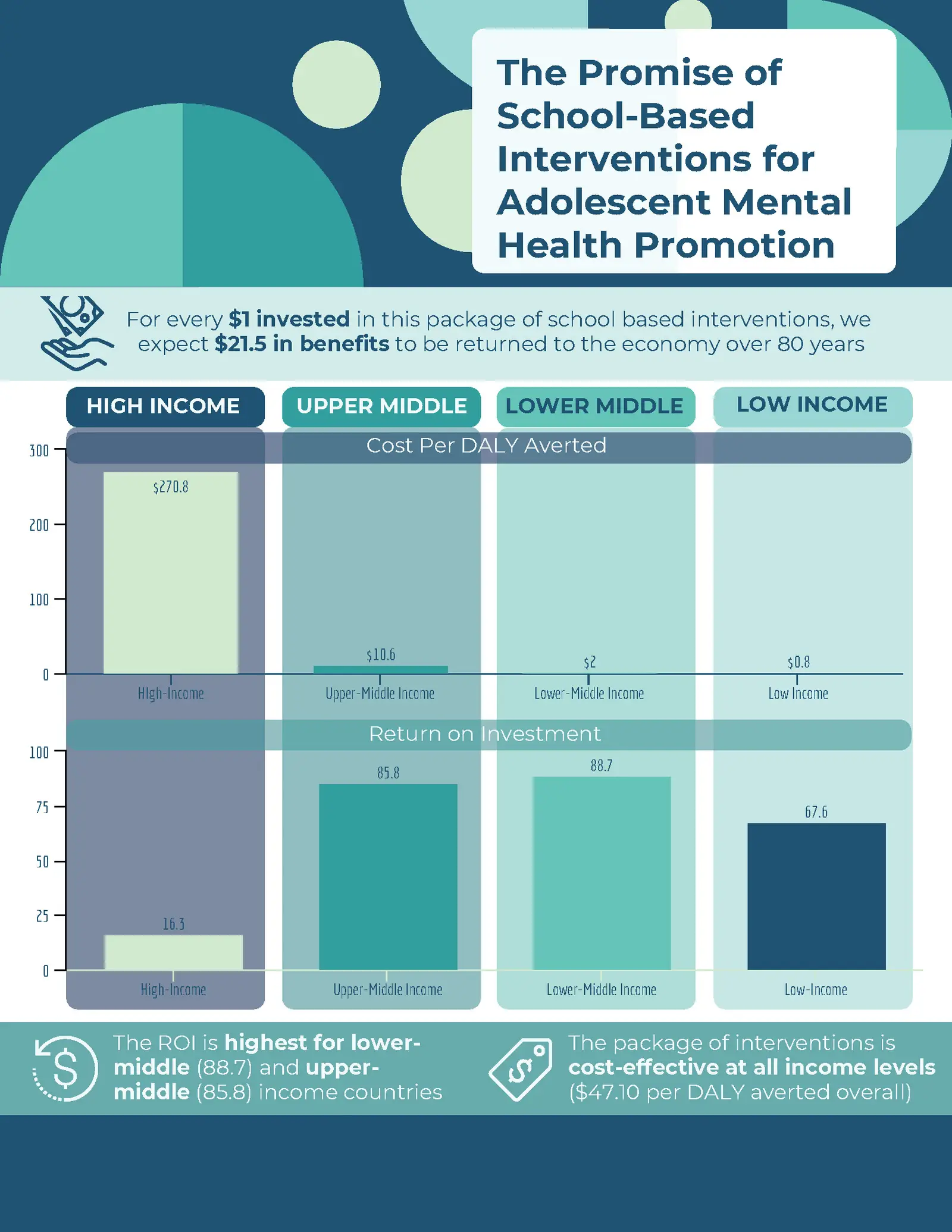
Our findings suggest that countries will experience a significant economic return on investment of implementing this package of interventions. We found the global ROI to be 21.5, meaning that for every $1 invested in the package, we expect $21.50 in benefits to a country’s economy over an 80-year period. The ROI is highest for lower-middle (88.7) and upper-middle (85.8) income countries due to lower costs of labor.The cost per disability adjusted life year (DALY) averted is $47 overall, and below $11 for LMICs.
Cost per DALY averted is a measure that estimates the ratio of the cost of an intervention to the associated health benefits, in terms of reductions in mortality and morbidity. For comparison, community management of severe acute malnutrition is estimated to cost $26-39 per DALY averted, and nutrition education in childhood $100 per DALY averted. An intervention is typically considered cost-effective if the cost per DALY averted is between one and three times a country’s per capita income, making this package very cost-effective at all national income levels.
National Adolescent Mental Health Investment Cases
This intervention package demonstrates a strong ROI that compares favorably to other child health interventions. The package of school-based interventions is therefore a cost-effective option for governments to address unmet mental health needs among their young populations and to avert the adverse health, social, and economic impacts of mental disorders.
In many countries there are already health programs that are delivered in schools, and a strong recommendation is that governments leverage and further strengthen this inter-sectoral partnership between the health and education sectors to deliver these impactful programs and protect young people’s mental health. The high estimated returns on investment of these programs also suggest the potential value of developing and scaling up innovative interventions that work across other sectors to reach adolescents, including those who are out of school.
However, these innovative inter-sectoral partnerships must also be accompanied by strengthening mental health provision more generally to provide services that are more accessible and appropriate for adolescents at all levels of the system.
Based upon the encouraging results of our global-level analyses, we are now conducting a series of national investment cases that are tailored to the mental health needs and context of young people in India, Indonesia, Mexico, South Africa, and the United Kingdom. We are working with stakeholders in each country to assess the economic benefits of investing in adolescent mental health, develop country-specific evidence to inform decision making, and advocate for the implementation of these promising, cost-effective approaches. Together, we aim to assist countries to address the pressing issue of unmet mental health needs among adolescents in ways that are effective, cost-effective, and feasible.

Shining a Spotlight on Adolescent Mental Health in Low- and Middle-Income Countries
This earlier blog offers insights on evidence-based, accessible, and engaging mental health interventions for adolescents in low- and middle-income countries.