Presented by Leslie Greenwald, chief scientist and vice president at RTI International, at the Health Affairs and National Pharmaceutical Council Forum on Health Spending.
For more than 30 years, the US has continued to spend larger proportions of our sizeable GDP on health care. As part of a research initiative supported by RTI Health Solutions and RTI International, I and other researchers investigated factors driving spending outside and inside the US to assess US spending on health care relative to other developed countries.
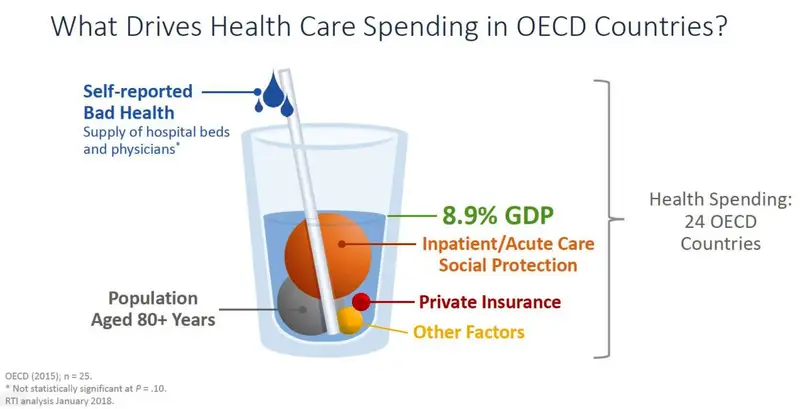
To illustrate, let’s first think of health care spending as a glass of water. In our first example, the fill line on the glass of water is at 8.9%. This represents the percentage of GDP spent on health care for 24 member-countries of the Organization for Economic Co-operation and Development (OECD) excluding the US.
In the following figure, different sized spheres represent factors that drive health care costs. We see that inpatient/acute care and social protection comprise the lion’s share of spending in OECD countries when the US is excluded.
Using this same approach, we then can assess factors driving health care costs in the US.
The clear difference between these two perspectives can be seen in the figure below. There is a lot more water filling up the US glass of water. This is because the US spends a much higher percentage of GDP on healthcare.

There are some similarities between the US and other OECD countries, such as poor health being associated with lower GDP spending. However, most of the other factors that get the US to the fill line are different. For the US, total GDP is by far the most important factor, followed by the percentage of the population aged 80 and older.
Based on our analyses, only a few factors really drive health spending when measured by the percent of GDP. Total GDP is the largest driving factor predicting US health care spending; it's not a major driver outside the US. Even when the factors are the same – such as percent of the population aged 80 and over – they matter to a different degree.
If the drivers of spending are economic, demographic, and social constructs, what does this mean? How do US wealth and these high-level constructs drive high US health spending? One way to understand these relationships is to look at recent policy debates and the policy norms our wealth allows us to adopt.
Health care reform efforts have found a clear preference for competing private health insurance versus government-run systems, which fragments the risk pool and raises costs. Health care reform that limits choice, or imposes rationing, in any way is a non-starter. Even the extensive Affordable Care Act places little or no responsibility on patients for the consequences of their health habits or compliance with prescribed medical directions. This contributes to high costs.
Medicare is considered nearly untouchable. While a very worthy and efficient program, it has created the only US demographic group, which we see in the driving factor of a population over age 80, that has nearly universal health insurance coverage. The aged are a highly insured and high-cost population, while a not-insignificant portion of the US is uninsured or underinsured. This approach to insurance coverage also contributes to high costs.
After many years of tracking US health spending outliers, unsustainable levels of spending seem remarkably sustained, and nearly constant health care reform debate hasn’t budged US spending downward. Maybe focusing on US health care spending as a percentage of GDP isn’t really the right focus anymore. Maybe future health care reform might be more productive if we shifted our focus from how much we spend to how and where we spend our health care dollars – however many dollars we have.

